
by Jennifer Wolkin | Jul 4, 2018 | Blog, Mindfulness, PTSD, Wellness
There is research that those experiencing PTSD reported improved well-being in response to poetry therapy. This might be the case because a hallmark of having experienced trauma is the subsequent difficulty processing the experience, which results in avoiding and suppressing associated emotions/memories.
Poetry therapy has provided an outlet for those suffering with PTSD to start to integrate many of these feelings, and even more so, to start to reframe the traumatic experience.
Poetry therapy itself is a bit abstract to describe, but there are a few ways to engage with it. Here is a multi-model poetry therapy practice developed by Nicholas Mazza, the founding and continuing editor of the Journal of Poetry Therapy.
According to Mazza’s model, poetry therapy involves three main components:
- Receptive/prescriptive: This part of therapy involves the clinician/therapist reading a poem out loud, and then subsequently encouraging the client to react to it, either verbally, non-verbally, or both. The therapist might even prompt: “Is there a particular line in the poem that resonated with you?”, or “I noticed you started to become teary-eyed when I read this line…”
- Expressive/creative: This entails actual creative writing. The therapist promotes stream of consciousness writing that might aid in discovering blocked emotions, parsing felt emotions, or retrieving memories that are difficult to articulate. The therapist might offer a prompt to help someone get started.
- Symbolic/ceremonial: This includes working with metaphor/simile to help further explain emotions that are hard to describe in a more literal sense. The ceremonial part may consist of writing a letter to someone they may have lost and then burning it.
The efficacy of poetry therapy is still being studied. Most of the empirical evidence for its effectiveness comes through James Pennebaker’s (a pioneer in the field of Positive Psychology) work in the therapeutic use of expressive writing. His studies have indicated that the use of expressive writing, even for as little as 15 minutes over the course of 4 days, resulted in positive health effects. In addition, his initial work dealt with the use of expressive writing to heal wounds from traumatic stressful events.
One case in point is that in the aftermath of 9/11, poetry was utilized as a healing mechanism. According to a New York Times article on October 1, 2001:
“In the weeks since the terrorist attacks, people have been consoling themselves—and one another—with poetry in an almost unprecedented way … Improvised memorials often conceived around poems sprang up all over the city, in store windows, at bus stops, in Washington Square Park, Brooklyn Heights, and elsewhere. …”
In some ways poetry gives us the way to speak about the unspeakable. It is more and more common for those suffering with medical challenges to write their story, many times in poetic form, to aid in their own healing. As always, it is crucial to note that just like with mindfulness approaches to trauma, poetry therapy is most often used in conjunction with other therapies.
On a personal note, I’m particularly drawn to this type of therapy and recently started studying for my MFA at Queens College. I am touched by the profound pain that is both individually and collectively felt, how this pain can displace someone from others and their selves, and yet, the profound capacity for resilience, healing, and growth. Aside from writing my own work, I hope to employ poetry as a technique to help my clients say what they couldn’t otherwise say.
Here’s an example of a poem that I recently published in the British Journal of Medical Practice in this vein:

by Jennifer Wolkin | Mar 12, 2018 | Blog, Brain Health, Five to Thrive, Mindfulness, Stress, Wellness
Live your best life: Mindfully control your brain’s reaction to stress
Did you know that the brain’s “stress center,” the amygdala, shrinks post mindfulness practice? In addition, the functional connections between the amygdala and the prefrontal cortex are weakened. This allows for less reactivity to life’s basic stresses, and paves the way for higher order brain functions to be strengthened (i.e. attention, concentration, etc.)

The impact that mindfulness exerts on our brain is borne from routine: a slow, steady, and consistent reckoning of our realities, and the ability to take a step back, become more aware, more accepting, less judgmental, and less reactive. Just as playing the piano over and over again over time strengthens and supports brain networks involved with playing music – mindfulness over time can make the brain, and thus, us, more efficient regulators, with a penchant for pausing to respond to external stimuli instead of mindlessly reacting.
The amazing thing about mindfulness is that you can apply it to any action you engage in on a daily basis; cooking, cleaning, walking to work, talking to a friend, driving – or even drawing or coloring!
Why coloring? Well, for one, we all need to embrace our inner child! As adults, we don’t do enough coloring, or any type of play for that matter. Did you know that play can help reduce stress? Also, believe it or not, coloring utilizes areas of the brain that enhance focus and concentration, and nurturing attention is one of the mechanisms by which mindfulness leads to well-being.
That is helpful, because when we are engaged “on purpose” in a particular task, by focusing on it instead of remaining on autopilot, then our negative and unhelpful thinking seems far away (i.e. isn’t on our minds!) Our minds literally can’t focus on both at the same time.
Yet, it should not be seen as just a distraction from really dealing with our “problems”. By engaging in this exercise, we can continue to deepen our ability to be mindful and train our mind to stay in the present moment rather than habitually straying into unhelpful thoughts about the past or future, to rather stay non-judgmentally present to our every sensation as it unfolds. In this way, we are better equipped to calmly approach our anxiety and parse out if it is a real or imagined stress.
How to practice mindful coloring:
- Start with colored pencils, or crayons or any other drawing/coloring tool that feels right to you.
- Take a moment to notice the feeling of these instruments in your hand. Their weight, texture, the engineering that went into their creation…
- Then, listen to your gut, and start to color without too much thought about it. Don’t analyze your drawing, rather, just let what comes organically come. Try not to edit.
- If you want, you can print multiple pages so you can do this over and over again.
- See if you can focus also on the act of coloring itself as you are engaged in it. Here are some cues for you:
- How does your hand move across the page? You might even want to spend some time following it.
- How do the different strokes look? Notice the difference between using the sharp edge vs. the side of the pencil.
- How do the different colors (if you are using multiple colors) add to the different parts of the image?
- Notice, without judgment, as your drawing unfolds.
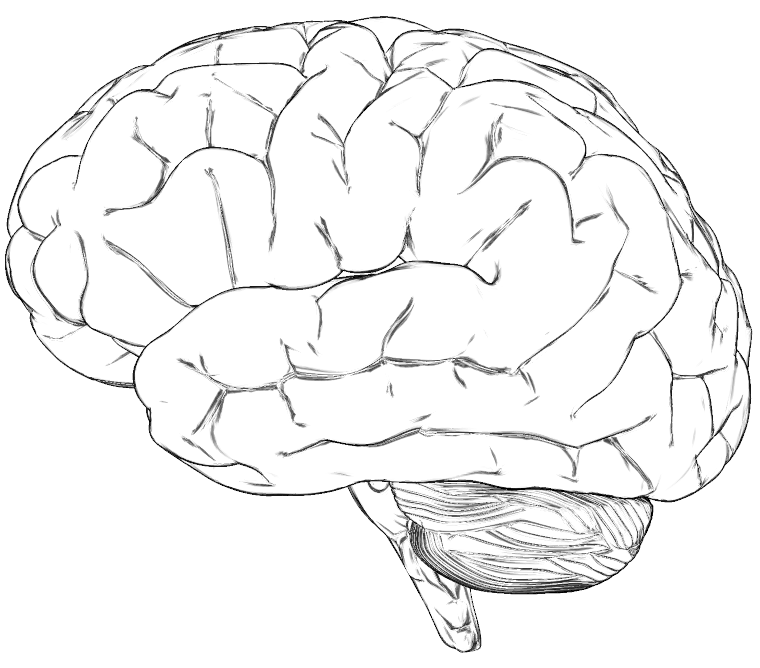
What does your unique brain look like?
In my ‘The Grand Conductor’ packet, we go through the biology of the brain, as well as the latest research on how to keep it in tip-top shape, but at the end of the day, it’s important to remember that we’re just brains studying brains. We’re limited in our understanding of the brain by the virtue of the very thing we’re using to study it!
In addition, just as every individual is unique, so is each brain different from the next, and, moreover, constantly changing as we age! So, let’s all open our minds (see what I did there?) and learn more about ours, and each other’s, unique brains.
Print out the brain image below and color it in however you please! Remember to try to practice staying mindful during the process. Let it reflect the latest brain science (learn more from the infographics at the bottom of this blog!) or let it reflect your own personal understanding of self. Whatever you decide – Let your mind soar! Keep in mind, it’s not about being an artist, in fact, no artistic skill is necessary. Just dive in and notice, again, without judgment, what the process is like for you. I’m going to do this as well, and share it on my social media pages, so stay tuned!

When you are finished, please, #ShareYourBrain on social media and tag @BrainCurves!
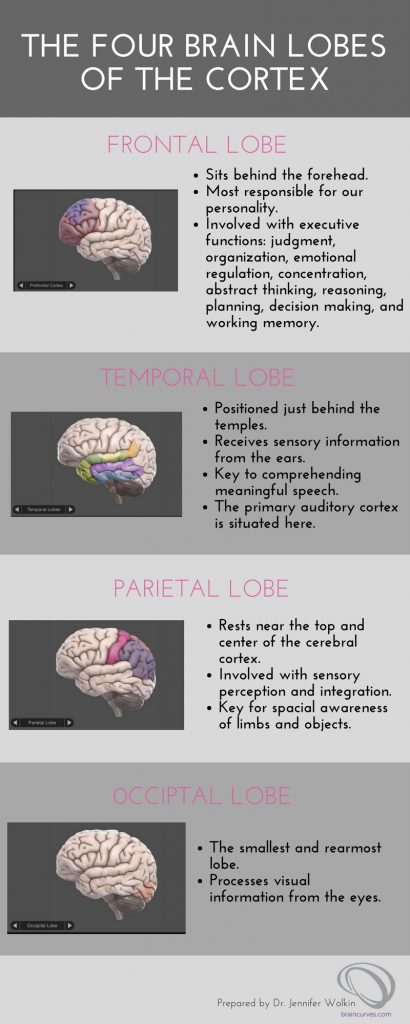
BRAIN EVOLUTION, ANATOMY & PHYSIOLOGY, AND WELLNESS INFOGRAPHICS


by Jennifer Wolkin | Apr 23, 2017 | Blog, Five to Thrive, Mindfulness, Relationships, Stress, Wellness
This blog post originally appeared on Mindful.org

An Early Account
In the 1950’s Dr. Thomas Almy, a prestigious gastroenterologist, snapped a picture of a live colon responding to the proverbial “butterflies in the stomach.”
Dr. Almy invited a student to take part in an experiment where he used a sigmoidoscope to look inside the student’s rectum and colon. A bystander complicit in the experiment said something about cancer of the colon. Upon hearing this, the student concluded that he must have cancer, at which time his colon started to change color, tense up, and contract rapidly. When the student was reassured that cancer was not his diagnosis, his colon regained its natural color, and relaxed.
This experiment paved the way for a deeper understanding of the visceral processes behind our gut-wrenching experiences. Getting butterflies before a big test or nausea right after a breakup: those feelings are much more than anecdotal. It’s a physiological reality that our emotions and stress physically impact our gut.
The Brain-Gut Axis and Stress
One of the major breakthroughs in understanding how the central nervous system (CNS) and the gut communicate was the discovery of the enteric nervous system (ENS). The ENS, sometimes called the “second brain,” is a complex system of about 100 million nerves found in the lining of the gut. Both of our brains, so to speak, are in constant dialogue and speak in many “languages” as they send signals to and fro via neural and endocrine pathways that collectively have been dubbed the “Brain-Gut Axis” (BGA).
The BGA plays a prominent role in our overall wellness, and there is significant evidence that it’s susceptible to stress. The route to BGA dysregulation has many avenues, all of which make the gut more vulnerable to disease.
Stress-induced changes in the physiological functions of the gut include changes in: gut motility, mucosal permeability, visceral sensitivity, gastric secretion, and the gut microbiota. Changes to gut microbiota is called dysbiosis, which may lead to disease. Many of these stress-induced changes account for the symptoms seen in many gastrointestinal disorders.
Functional Gastrointestinal Disorders (FGIDs): When the Gut Acts Up
In my clinical practice, evidence of the BGA is most visible in the functional gastrointestinal disorders (FGIDs): cases when the gut is acting up and there’s no obvious physical cause, like a tumor or bowel obstruction, for example. This does not mean that an FGID is all in one’s head, however. A more precise conceptualization is that stress influences the actual physiology of the gut. In other words, psychological factors can impact upon physical factors, like the movement and contractions of the GI tract, causing inflammation, pain, and other bowel symptoms. These disorders often significantly reduce quality of life.
FGIDs include the better-known irritable bowel syndrome (IBS) and the lesser-known small intestinal bacterial overgrowth (SIBO). Given their functional nature, they continue to be difficult to treat, and often require GI doctors to use multiple treatment modalities and make referrals to other clinicians, including psychologists.
A Vicious Cycle
To be clear, the brain-gut connection is complex. For one, it is bidirectional; just like a stressed brain sends signals to the gut, a troubled gut sends signals to the brain, putting someone at greater risk for anxiety and other neuropsychiatric difficulties. Parsing which came first, the stress or the gut distress, becomes challenging and most often this bidirectionality between enteric and central nervous systems is a vicious cycle of great discomfort.
Just like a stressed brain sends signals to the gut, a troubled gut sends signals to the brain, putting someone at greater risk for anxiety and other neuropsychiatric difficulties.
On top of that, many of the FGIDs become chronic conditions, which pose a stressful physical and psychological burden. Many of the patients I treat come see me because having a disorder like IBS primes them for stress that maintains the original symptoms. For example, while stress is a clear player in the origin of FGIDs, “gut-focused” thoughts, emotions, and behaviors start to create stress that reinforces the underlying pathophysiology (i.e., slows motility, visceral pain). For example, my patients with FGID have become hyper-vigilant of their heightened visceral pain and then begin to catastrophically appraise their abdominal sensations. Also, their quality of life starts to significantly decrease, many times leading to anxiety and depression.
Many of the patients I treat come see me because having a disorder like IBS primes them for stress that reinforces the original symptoms.
A SIBO Story
I’ve learned about the FGIDs firsthand. I have a deeply personal connection to the BGA, and it serves to enhance my professional passion and expertise on the subject. In the winter of 2013, I experienced a feeling of pressure in my stomach after every meal. I felt visceral pain, and it felt difficult to empty my bowels. My heart felt fiery. I wasn’t just bloated—I looked pregnant. I had a belly the size of six-month gestational equivalence.
I wasn’t just bloated—I looked pregnant. I had a belly the size of six-month gestational equivalence.
I was otherwise healthy, and thankfully so, and the onset of symptoms was anxiety provoking. After a multitude of tests ruled-out anything life threatening, I took a hydrogen breath test that my GI specialist said was indicative of small intestinal bacterial overgrowth (SIBO).
I had never heard of it before, so I began to just refer to myself as a “digestive mess.” It definitely felt like a mess, as SIBO had nonchalantly decided to go camping in my gut, like a pesky parasite sucking the life out of every ounce of normal flora to be found. Camping: as in pitching tents, starting fires, and sleeping in the dark hollows of my alimentary organs (i.e., my gastrointestinal tract).
This was my up close and personal reckoning with just how much stress was taking over my mind—and body. SIBO was a wake-up call to inspect my habitual patterns of thinking and behaving that were adding to my stress levels over time.
This was my up close and personal reckoning with just how much stress was taking over my mind—and body. SIBO was a wake-up call to inspect my habitual patterns of thinking and behaving that were adding to my stress levels over time. These patterns weren’t “bad” per se, they were just not serving my wellness. It is hard to pinpoint any one stressor, or any one pattern that contributed to SIBO. In retrospect, it was probably an accumulation of stress that I carried with me during a grueling postdoc. Postdoc was an extraordinary experience that afforded me first-class training. Yet, I pushed myself without taking the time to rest. I can still recall one of my supervisors saying that “postdocs” never get sick, or if they do, they sweat through it, and suck it up. All I could think then if I needed a break was “I am such a failure.” I think I carried this line of thinking with me as I embarked on the first phase of my career post-training. I kept going without rest, and if I needed a break I’d once again hear the stress-inducing voice in my head reminding me of what I thought was my inadequacy.
It is hard to pinpoint any one stressor, or any one pattern that contributed to SIBO. In retrospect, it was probably an accumulation of stress that I carried with me during a grueling postdoc. Postdoc was an extraordinary experience that afforded me first-class training. Yet, I pushed myself without taking the time to rest. I can still recall one of my supervisors saying that “postdocs” never get sick, or if they do, they sweat through it, and suck it up. All I could think then if I needed a break was “I am such a failure.”
SIBO was a wake-up call, albeit a very uncomfortable one. So uncomfortable that I began to resent my body, avoiding social engagements, and hyper-focusing on my symptoms. The heaviness I physiologically felt in my core became a psychological burden, and I became depressed, until I finally realized that by calling myself a “digestive mess” I was colluding in the maintenance of my pain.
4 Ways to Treat FGIDs Using the Mind
Since multiple components, including physiological, affective, cognitive, and behavioral factors are associated with FGIDs, an integrative approach to treatment is prudent. The research indicates that psychological interventions have been successfully applied. More specifically, a large number of randomized controlled trials suggest that cognitive behavioral therapy (CBT), biofeedback, relaxation techniques, and mindfulness meditation are effective psychological interventions for FGIDs.
1) Cognitive Behavioral Therapy
Cognitive Behavioral Therapy is based on the idea that sometimes people engage in habitual thinking patterns that are founded on a skewed perception of their experiences or unhelpful, “distorted” thinking. It’s an inquiry-based approach that asks people to take notice of their mood changes and the habitual patterns of behavior they engage in.
CBT is the most studied psychological intervention vis-à-vis FGIDs, and most studies were conducted with IBS populations. Many people with IBS engage in unhelpful thinking styles related to their actual symptoms, which then impact upon their moods and behaviors. For example, imagine a scenario during which someone with IBS is certain that eating out in public means they will absolutely have diarrhea. The thought creates anxiety, which might actually lead to autonomic arousal that could potentially trigger diarrhea. Eating out is now linked to having diarrhea and so eating out is likely avoided. CBT treatment would first be geared toward helping someone identify this pattern of thinking, feeling, and behaving. Then it would be utilized to help someone learn to challenge this unhelpful thinking and develop healthy active coping skills.
One study conducted over twenty years ago focused on the impact of CBT on IBS by randomizing 34 patients to eight weeks of cognitive therapy, a self-help support group, or a waitlist control. The results indicated that post-treatment the cognitive therapy group showed a significant reduction in gastrointestinal symptoms, as well as significant improvement on measures of depression and anxiety when compared to both the support group and waitlist control paradigms. These results were maintained at a three-month follow up.
A recent study, published in January 2017, looked at the effects of a 12-week course of face-to-face CBT on 18 subjects with IBS. Results indicated a decrease in self-rated visceral sensitivity, as well as associated psychiatric symptoms. The authors of the study attributed the results to increased ability to cope with IBS symptoms.
2) Relaxation Techniques
In 1975, Herbert Benson, a physician at Harvard, introduced the concept of the relaxation response. It is the physiological opposite to the fight or flight response. In this way, stress management can be achieved by dampening the effects of the sympathetic nervous system’s “fight or flight” arousal mechanisms by activating our parasympathetic nervous system through relaxation techniques.
Research has suggested that practices like meditation, yoga, and prayer, which elicit the relaxation response, alleviate stress and anxiety’s physiological counterparts, which as we now know, can impact gut motility and induce dysbiosis.
A pilot study from Harvard University affiliates Benson-Henry Institute for Mind Body Medicine at Massachusetts General Hospital and Beth Israel Deaconess Medical Center was designed to investigate whether meditation, a relaxation-response-based intervention could reduce negative symptoms and improve quality of life in patients with IBS and irritable bowel disease (IBD). Forty-eight patients with either IBS or irritable bowel disease (IBD) took a 9-week session that included meditation training, and the results showed reduced pain, improved symptoms, stress reduction, and the change in expression of genes that contribute to inflammation.
3) Biofeedback
Biofeedback uses computerized technology to help someone learn to control or manage the body’s response to stress. Sensitive instruments are used to measure physiological processes, like heart rate variability and/or muscle contractions, for example, with the purpose of “feeding back” the information to someone so they can learn to control them.
In terms of FGIDs, biofeedback’s effectiveness has mostly been investigated in those experiencing functional constipation. In this case, biofeedback is used to help someone tune in to a propensity for paradoxically contracting the pelvic floor muscles during bowel movement (often referred to as pelvic floor dyssynergia (PFD), and then to train someone to relax these muscles instead.
One study compared the effects of five weekly biofeedback sessions with those of laxatives plus counseling in patients with severe PFD. The researchers studied overall satisfaction with treatment, symptoms of constipation, and pelvic floor physiology. At six months, improvement was reported in 80% of patients in the biofeedback group vs. 22 % in the other group. Results were sustained at 12 and 24 months post-treatment. More specifically, biofeedback produced a greater reduction in straining, a greater reduction in the sensation of incomplete evacuation, a greater reduction in abdominal pain, and reduced use of suppositories. Since the study clearly indicates the benefits of five biofeedback sessions vs. continuous laxative use, it’s become the gold standard for treatment for this type of functional constipation.
4) Mindfulness Meditation
John Kabat-Zinn, the pioneer of mindfulness meditation’s use in Western psychological interventions, proposes that mindfulness is a state of greater awareness cultivated by paying attention on purpose, in the present moment, and without judgment. This definition reflects mindfulness’ positive impact upon sensory, cognitive, and emotional processing through cultivating purposeful, present-moment focus on experiences without the added judgment and evaluation often projected onto them. Since FGIDs are often maintained by the stress burden induced by the narrative that is created about the symptoms—a narrative that is rooted in judgment—mindfulness meditation has recently been studied and added to a growing list of possible psychological interventions for FGIDs.
One particular study in the Journal of Behavioral Medicine, looked at the impact of mindfulness training based on the MBSR program developed by Kabat-Zinn, on the quality of life of 39 women with IBS. As compared to a control group, the women who received the training experienced a significant attenuation of symptoms and an increase in quality of life.
More specifically, the mindfulness training cultivated a less reactive mindset toward potentially distressing thoughts, emotions, and sensory experiences. As the women were able to just witness their visceral sensations without catastrophically appraising them, anxiety was reduced, pain was attenuated, and they even started to think they had the potential to successfully cope with their symptoms.
Mindfulness for My SIBO Case
I personally looked toward mindfulness meditation to help me sit through a lot of the discomfort from SIBO. I repeatedly practiced sitting with the sensory experience of my symptoms without the added judgment. The anger toward my body for betraying me was slowly replaced with a compassion for what it was enduring.
The anger toward my body for betraying me was slowly replaced with a compassion for what it was enduring.
Overall, what I learned through my healing process, in a nutshell, is that given just how clear it is that emotional and psychosocial factors can trigger symptoms in the gut, I needed to make some lifestyle changes. So I did, and I still do. When we have engaged with certain unhealthy thoughts, feelings, and behaviors for a long time, the path toward wellness takes extra patience, perseverance, time, and trust. Nothing about the path is easy. Sometimes, it’s even disheartening. Always, it’s worth the chance to thrive.











